Gout is a disease that falls under the category of inflammatory arthritis diseases. It is a form of arthritis capable of causing severe, acute pain in affected joints. The pain might be constant, but it doesn’t necessarily have to be. Indeed, many patients experience gout pain on an intermittent basis, and it is even possible to experience the pain so infrequently that it is not associated with gout at all.
Some estimates suggest that one in every 50 UK residents have been affected with gout at some time or another. Furthermore, there could be many more cases left undiagnosed. However, the more we learn about the disease, the more we are coming to understand that it may be related to diet and lifestyle.
Direct Causes of Gout
When we talk about the causes of gout, we must discuss both direct and indirect causes. There is only one direct cause: the build-up of urate in the joints. Urate, also known as uric acid, is present in the human body due to the way food is broken down and utilised.
Uric acid is the result of substances known as purines. Those substances are broken down by the digestive system into usable and non-usable components. Uric acid is non-usable. The body attempts to flush it out as quickly as possible. Over time though, uric acid can build up. This results in crystals forming under the skin and within the joints. The crystals interfere with normal joint operation, thus causing joint swelling and pain.
As for indirect causes, studies suggest gout could be linked to:
- genetics
- excess weight
- alcohol consumption
- diet
- medications
it is also possible that gout is the result of an underlying medical condition. Diabetes, hypertension, and chronic kidney disease are the most likely suspects. All of these conditions can lead to an increase in uric acid. A gout specialist would be the most qualified clinician to make this sort of determination.
Signs and Symptoms
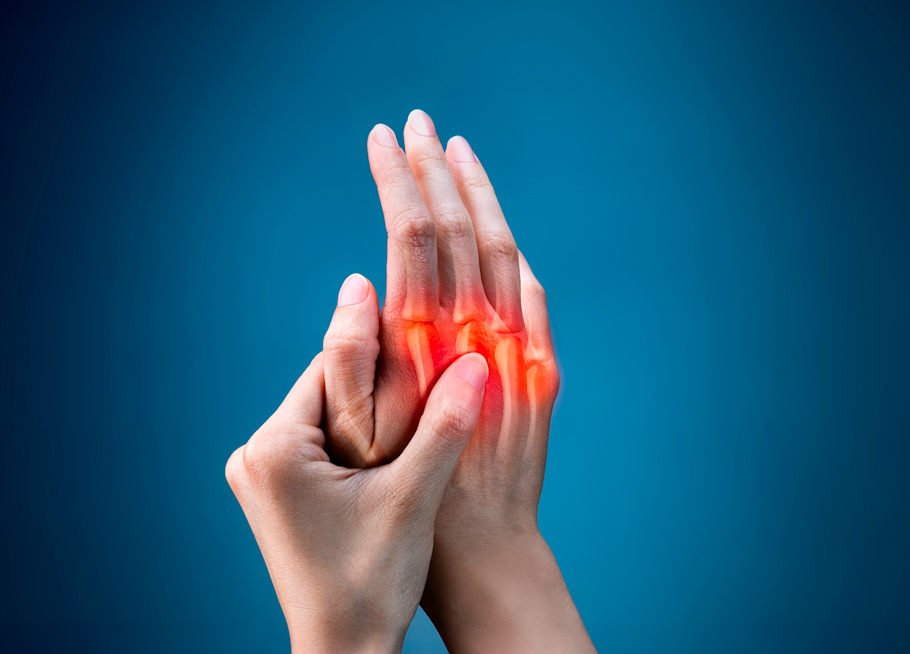
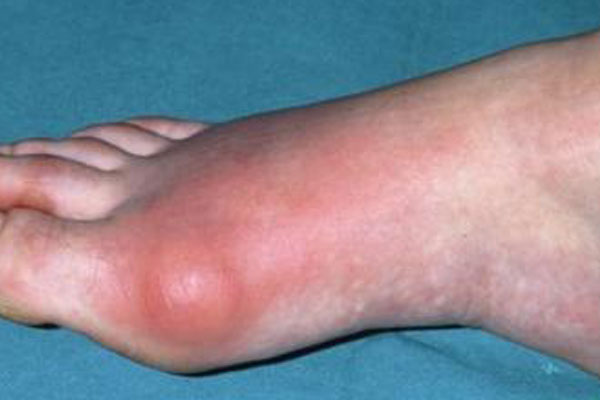
Gout normally presents as pain in one or more joints. The pain is often severe and acute, though different patients present with different levels of pain. Doctors look for symptoms like:
- severe pain in multiple joints
- pronounced joint swelling
- joints that feel hot and tender
- red, inflamed skin around affected joints.
A typical gout patient will notice the most significant pain in joints at the ends of affected extremities. This typically means fingers, toes, ankles, and knees. Although any joint can be affected, those at the ends of certain limbs seem to be more prone to uric acid build up.
How Gout is Diagnosed
The disease can be diagnosed by either a GP or a private consultant for gout. Doctors begin by asking pointed questions about symptoms. They also conduct a physical examination to look for joint swelling and inflamed skin. If gout is suspected, a couple of tests can be ordered.
There is a simple blood test that can identify excess uric acid in the system. A GP can conduct this test. Nevertheless, a blood test alone doesn’t confirm a gout diagnosis. It simply raises suspicion when high levels of uric acid are detected. For confirmation, a second test is needed.
This second test analyses joint fluid drawn from the patient’s affected joint. By viewing the fluid under a microscope, it is possible to see uric acid crystals. They are identified by their unique, needle-like shape.
Treating Gout
Knowing that the direct cause of gout is excess uric acid generally leads doctors to follow a multi-pronged treatment protocol. Doctors have three goals in mind: managing acute pain, reducing the likelihood of future attacks, and finding ways to reduce uric acid levels.
The first step is to manage acute pain through the use of painkillers and anti-inflammatory drugs. NSAIDs, steroids, and colchicine (a pain reliever) are common choices. Immobilisation is often recommended in especially severe cases.
The second and third avenues of attack are centred around changing lifestyle habits. For example, an obese patient will be encouraged to lose weight. Patients will be encouraged to avoid alcohol consumption and change their diets to reduce foods high in purines.
In general, the best way to address gout – beyond pain management – is to adopt a generally healthy lifestyle that includes a healthy diet and regular exercise. If underlying conditions are the cause, doctors will take them into account when prescribing lifestyle changes.
If you think you might be exhibiting symptoms of gout, see your GP or a private consultant for gout. Dr Naveen Bhadauria, private consultant rheumatologist, will be able to help you.
Article by Dr. Naveen Bhadauria